Male Breast Surgery (Gynecomastia) on Cape Cod
Gynecomastia is a condition where the male breast is enlarged. It is actually far more common than most men realize. A patient with this condition may have it in one breast only (unilateral gynecomastia) or have it in both breasts (bilateral gynecomastia).
Currently, there is no clear explanation of why this happens. While there certainly do appear to be some medications and drugs that can cause gynecomastia, there are many men who have not been exposed to these drugs that have gynecomastia. Exposure to steroids, marijuana, excess alcohol, or digitalis has been known to cause gynecomastia. A patient should stop using these items before surgery to see if this alone will correct the condition.
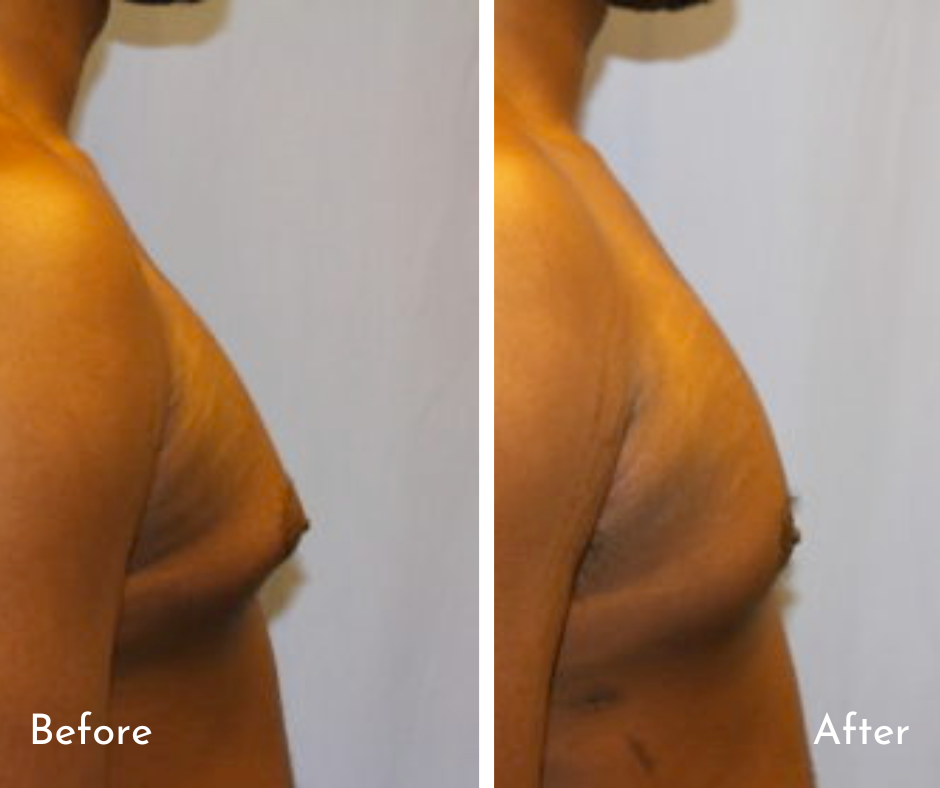
Types of Gynecomastia
There are two patterns of gynecomastia.
The first pattern (true gynecomastia) refers to an excessive amount of firm breast tissue beneath the nipple.
The second type (pseudo-gynecomastia) refers to a diffuse amount of fatty tissue throughout the breast.
The patient with the first type of gynecomastia tends to be a young male of appropriate body weight. The second type of gynecomastia pattern tends to be an overweight male. These patients tend to be of an older age group (over fifty). However, with today’s crisis of obesity, gynecomastia of the second pattern is now being commonly seen in younger men.
Who Is A Candidate For Gynecomastia Surgery
The more ideal surgical candidate for the correction of gynecomastia is the younger patient of ideal body weight, who has a small amount of extra breast tissue in one or both breasts. This is because his breast skin has more elasticity and therefore less chance of sag. In addition, this type of enlargement can usually be corrected without a large scar being placed horizontally across the breast. Dr. Loffredo and Dr. Jones usually perform the correction of true gynecomastia surgery on this type of patient by making a small incision around the areola and scooping out the excess breast tissue. While there is an incision on the breast, it is at the junction of the areola, and therefore less noticeable. Our surgeons typically use liposuction as well to provide for a better aesthetic result. Major reductions that involve the removal of a significant amount of tissue and skin may require larger incisions that result in more conspicuous scars. If liposuction is used to remove excess fat, the cannula is usually inserted through the existing incisions.*
What Are Other Methods Are There For Breast Reduction?
If your gynecomastia consists primarily of excessive fatty tissue, your surgeon will likely use liposuction to remove the excess fat. A small incision, less than a half-inch in length, is made around the edge of the areola – the dark skin that surrounds the nipple. Or, the incision may be placed in the underarm area. A slim hollow tube called a cannula, which is attached to a vacuum pump, is then inserted into the incision. Using strong, deliberate strokes, the surgeon moves the cannula through the layers beneath the skin, breaking up the fat and suctioning it out. In extreme cases where large amounts of fat or glandular tissue have been removed, skin may not adjust well to the new smaller breast contour. In these cases, excess skin may have to be removed to allow the remaining skin to firmly re-adjust to the new breast contour.*
In all situations where the patient is young and close to or at his ideal weight, Dr. Loffredo or Dr. Jones will carefully evaluate the patient’s medical history. If they feel that the patient needs to consult with an endocrinologist to rule out any hormonal problems or needs to have a mammogram to rule out breast cancer, then they will refer the patient to the appropriate medical provider. Dr. Jones and Dr. Loffredo always want to make sure before they perform any cosmetic surgery on a patient that there is no underlying medical problem causing the patient’s condition.
What Can I Expect Post-Op for Gynecomastia?
All gynecomastia patients will wear a surgical vest for three weeks. Dr. Loffredo or Dr. Jones will measure you for this vest, and they will supply you with two of them (one to wear and one to wash). All patients should plan on being seen the day after discharge from the hospital, as well as a few other post-operative visits. Our surgeons always provides you with enough pain medication to make you comfortable post-operatively. Patients will usually transition to Tylenol after 1 to 2 weeks post-operatively.*
Patients will need to plan on taking two weeks off from work or school to have this surgery. Patients can resume light exercise such as walking at about two weeks and be back on their full exercise regime at six weeks. Weightlifting will be allowed closer to the six-week period. All patients should discuss their resumption of activities with Dr. Jones or Dr. Loffredo to ensure their safety and proper healing.*
*Individual results may vary from person to person.


